Telemedicine & Digital Health
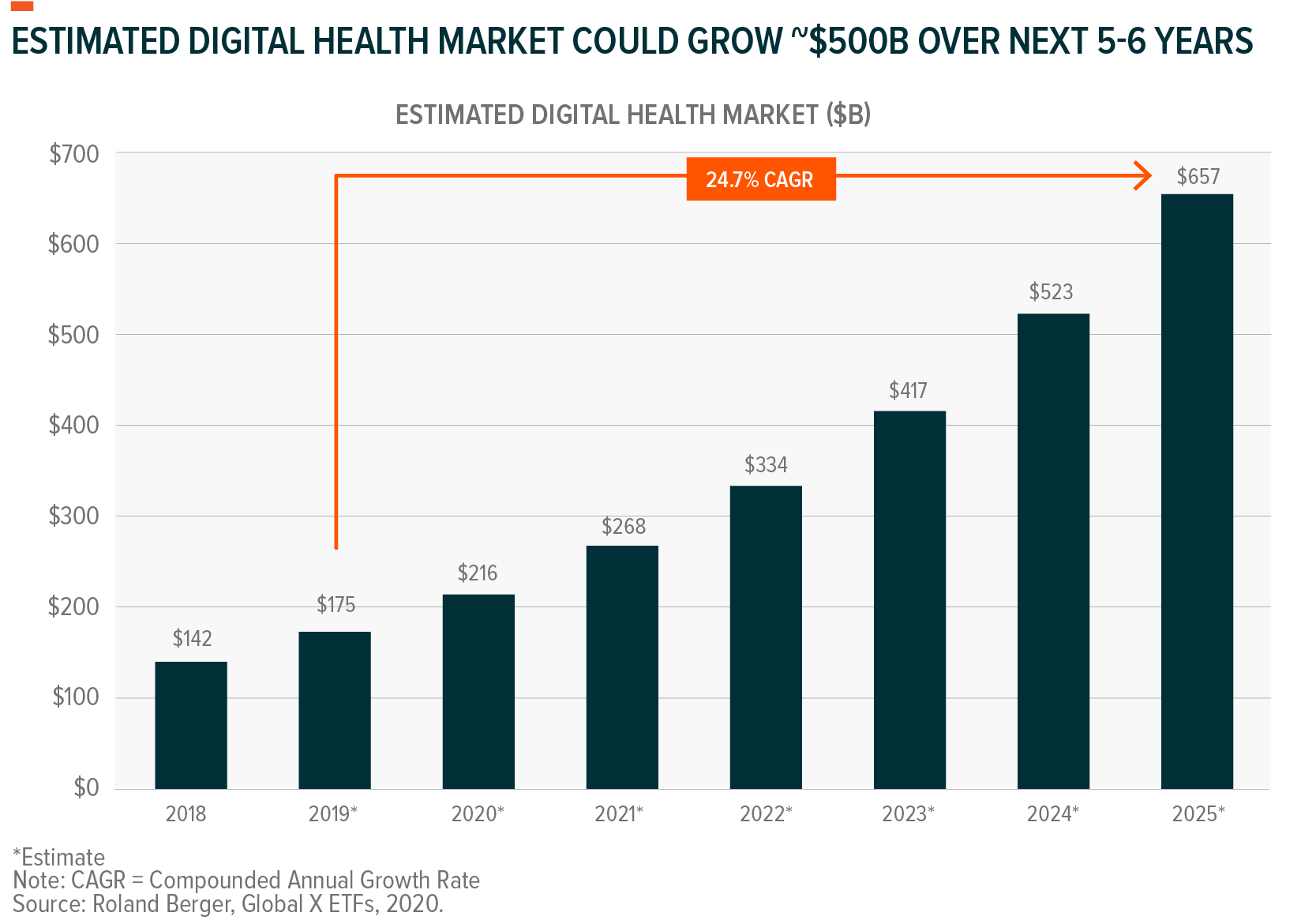
Telemedicine and Digital Health has received significant attention throughout the ongoing COVID-19 pandemic. With large swaths of the global population under stay-at-home orders, technology-based tools that facilitate remote communication with doctors and enable patient monitoring became critical.1 Some U.S. health care providers report that telehealth visits, defined as consultations in which a patient connects with a doctor via voice or video chat, increased by as much as 175x since the pandemic began.2 Additionally, the strain the pandemic put on all aspects of the global health care system highlights broader opportunities to modernize health care by more effectively leveraging technology and digitization.
Expanding Health Care’s Reach
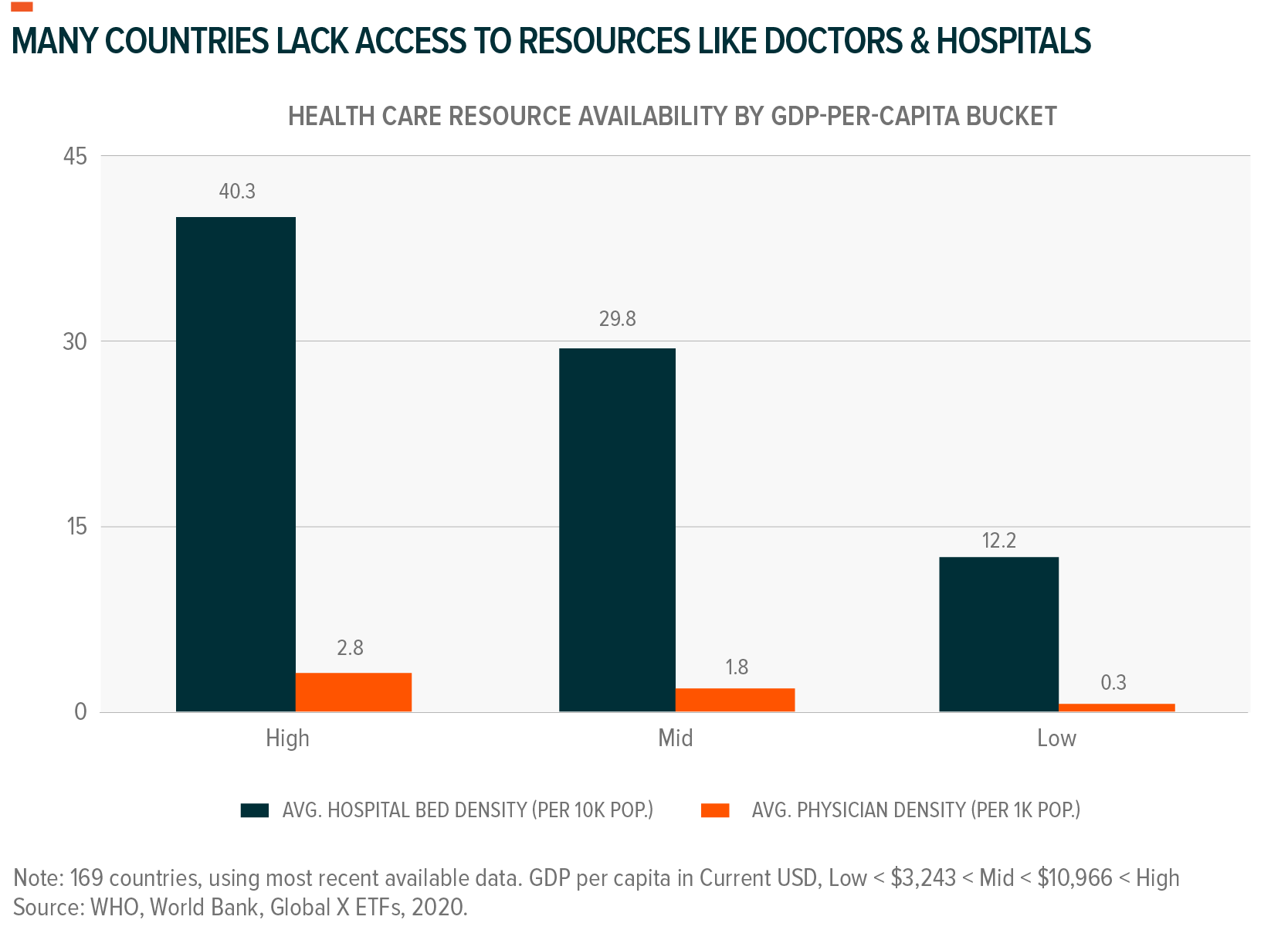
Half of the global population lacks access to essential health services.3 A portion of this is attributable to geographic location and physical distance from health care resources and/or professionals.4 Telemedicine can help expand essential care to these individuals.
Rural areas in the U.S., which saw 120 hospitals closures since 2010, have welcomed telemedicine and seen early successes.5 According to a recent survey conducted by NPR (National Public Radio), 24% of rural adults indicated use of telehealth, with 90% of those individuals noting satisfaction with the service.6 To the benefit of both individuals and health care systems, rural telemedicine adoption can limit the number of emergency room transfers from rural to more developed areas.7 Previous limitations to these services included lack of broadband access, but the FCC’s (Federal Communications Commission) July 2020 commitment of $200M to improve rural telehealth infrastructure should prove to be a tailwind to these services, as should broader rollouts of high speed internet and 5G technology.8
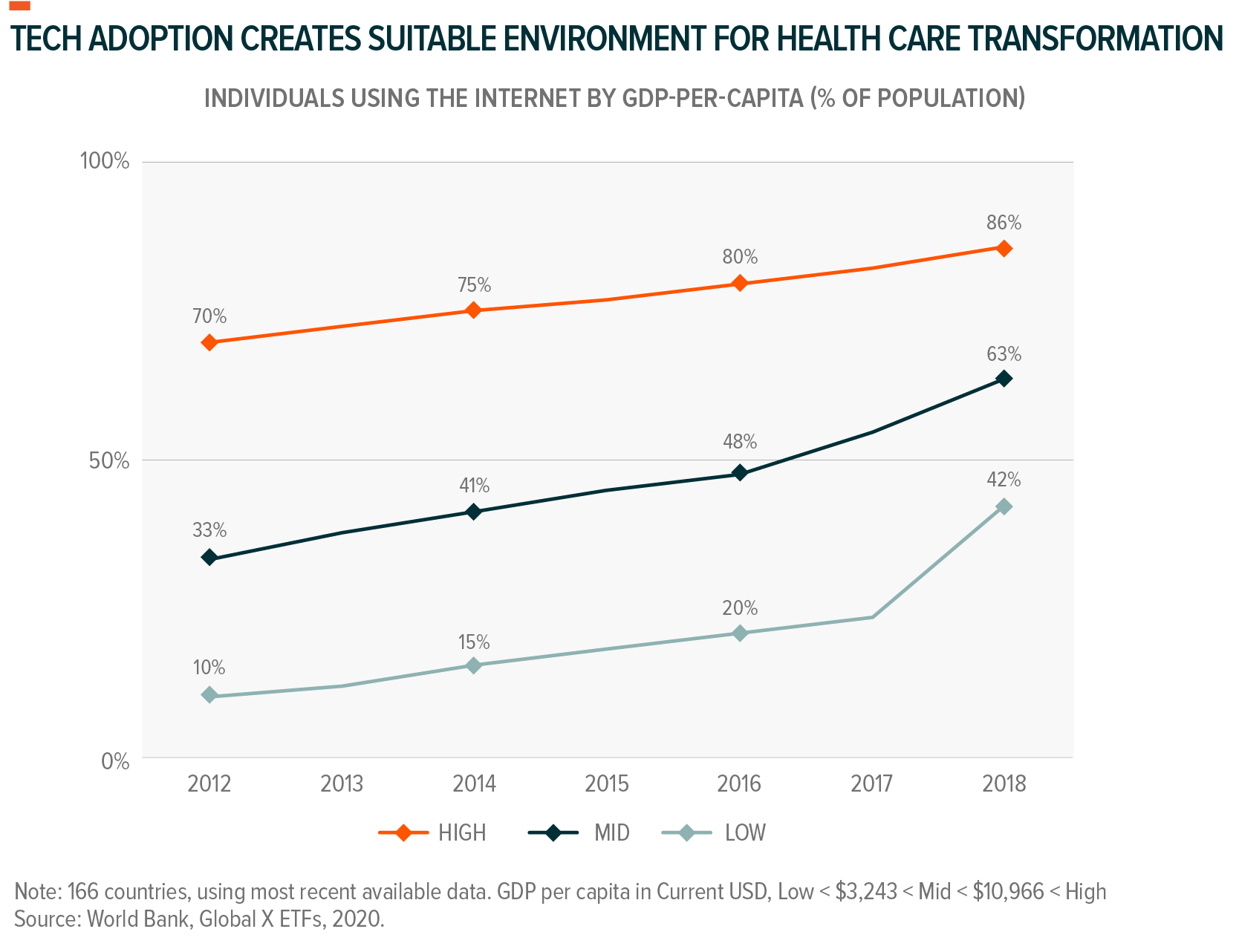
Similar opportunity for the technology lies in even more remote locations around the world. In sub-Saharan Africa – where skin ailments are common, but dermatologists are scarce – researchers established a mobile teledermatology service. Through their work, they diagnosed 49% of patients seen with inflammatory skin diseases and received positive feedback from 81% of local health care workers.9 Doctors Without Borders similarly implemented a telemedicine program in Somalia and, in one year’s worth of tele-consults, found that 56% of those consults added significant diagnoses and 25% caught life-threatening conditions.10 While many of these remote areas lack the connectivity infrastructure for full scale deployment of this technology as of now, global internet adoption continues to rise.
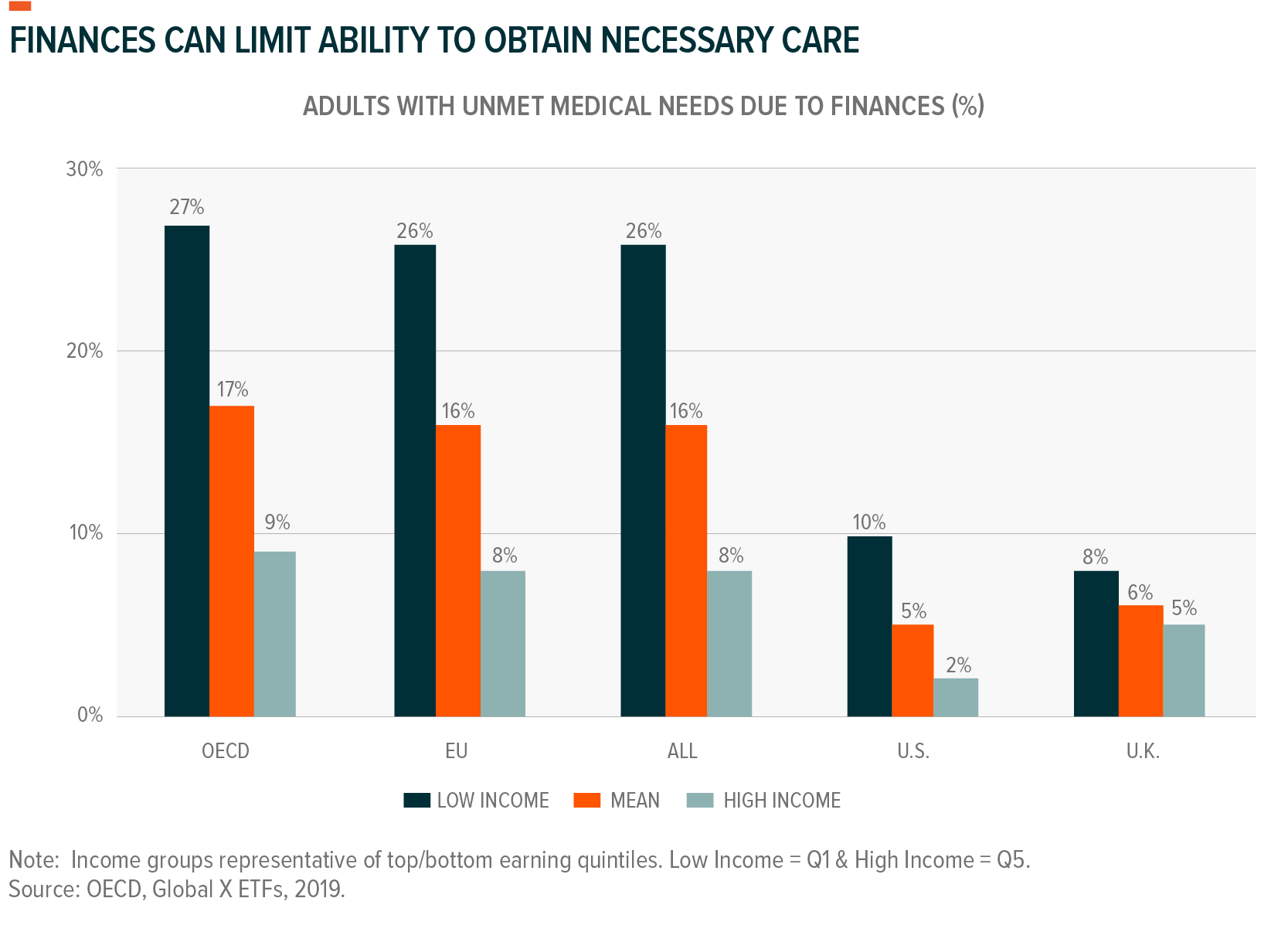
Economic constraints also contribute to individuals forgoing medical treatment. In OECD (Organisation for Economic Co-operation and Development) countries, 17% of adults indicate that financial considerations contribute to their unmet medical needs.11 Telemedicine can play a role in reducing these costs. In the U.S., health insurance provider Anthem reduced its co-pay for telehealth visits to $5, a stark contrast to the $25-35 charged for in-person primary-care visits.12 The immediate value from a one-off consultation is apparent, but the compounding cost-savings from ensuing follow-ups could result in savings that could positively affect patients’ indifference curves for seeking health care. In all, the U.S. Veterans Health association estimates $6,500 annual savings for each patient participating in telehealth.13 Additional savings can come from minimized travel costs. Between 1996 and 2013, the University of California Davis Health System found that telemedicine saved its patients $2.9 million of total direct travel costs and 9.0 years of transit time.14 And although affordability means lower per-use service costs for providers, the incentives presented by overall cost-savings, convenience, and meeting unmet needs drives usage and adoption, potentially more than making up for any lost revenue.15
Smart Treatments and Better Outcomes
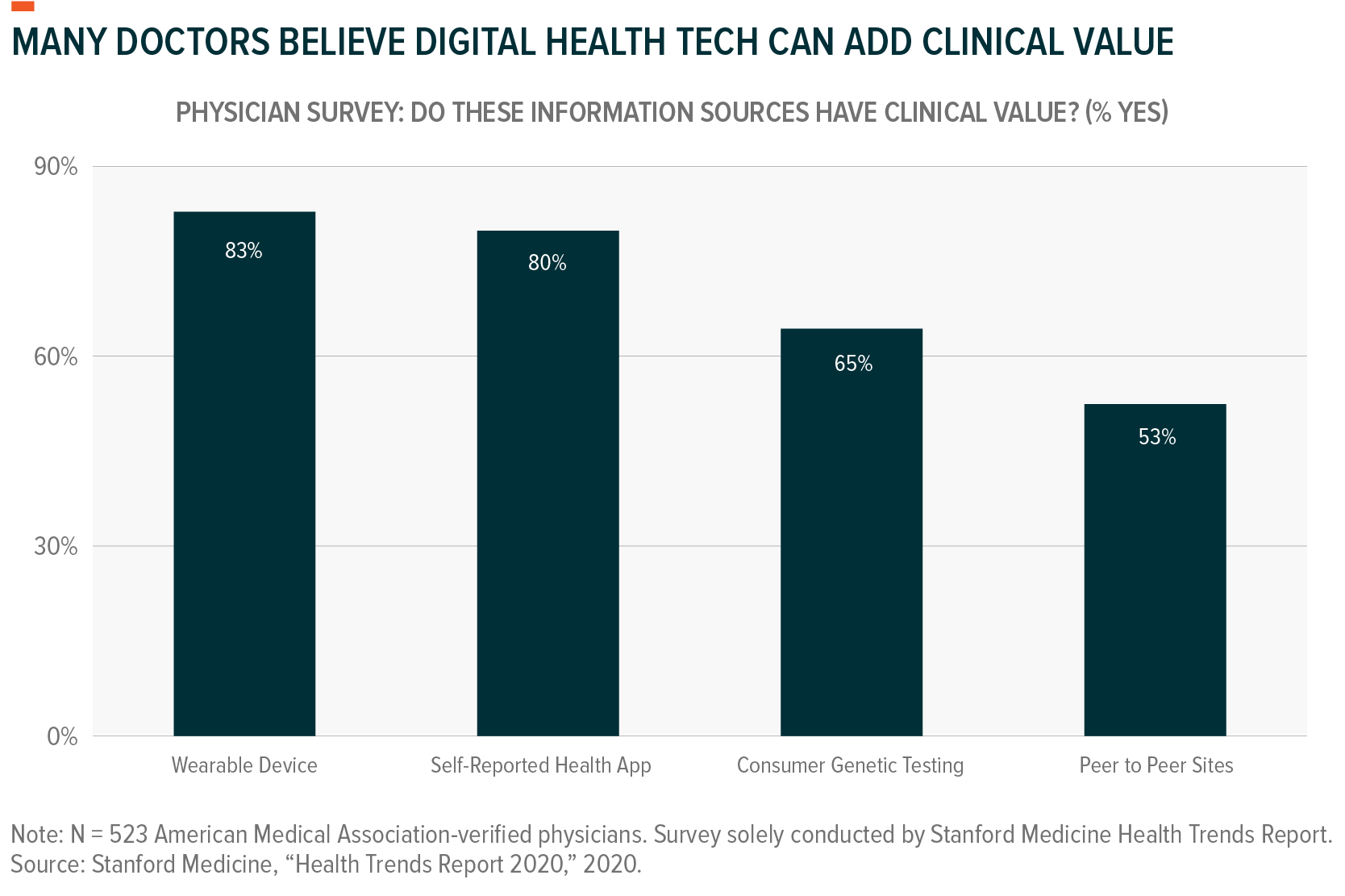
Digital health tools are revolutionizing the ways that providers care for patients, delivering novel solutions to enhance health outcomes across a variety of areas. Treatment adherence, or patients’ ability to follow through with medical advice and care, is one such area.
Treatment adherence is widely known as a primary impediment to the effective provision of care – less than 50% of patients demonstrate full adherence to provider-directed regimens.16 Some studies show that non-adherence causes around 125,000 deaths and up to 25% of U.S. hospitalizations each year.17 Telemedicine offers a potentially effective solution, by making communication with doctors more convenient and less expensive. This can prove especially valuable for chronic illnesses that require constant monitoring.
Sufferers of chronic heart failure (CHF), for example, require dynamic risk identification and timely intervention to manage their condition. In an analysis of congestive heart failure studies, researchers found that patients using telemedicine saw mortality decreases ranging from 15% to 56% compared to those not using telemedicine (across 18 of the 19 studies reviewed).18 A separate study looked at the efficacy of telemedicine in enforcing medication adherence in patients with severe mental illness. Results showed that after six months, the patient cohort using telemedicine was far more likely to be medication-adherent.19
Internet-of-Things (IoT) medical devices, connected wearables, and self-reporting mobile health applications further close the physical distance between providers and patients, allowing for monitoring away from traditional points of care. In 2017, the FDA (Food and Drug Administration) approved an ingestible sensor-equipped pill to treat schizophrenia, mania, bipolar I disorder, and depression in adults. The pill syncs up to a wearable patch, which then communicates with a smart phone to yield information around ingestion that can be useful to patients and providers.20
Beyond adherence monitoring, such technology can give doctors valuable information around their patients’ health from afar. Remote intensive care units (eICUs) contain myriad connected devices ranging from cameras, ventilators, and monitoring systems that track vitals like temperature, SpO2 (oxygen saturation), ECG (Electrocardiography), heart rate, blood pressure, and more. Data shows that these centers can contribute to a 15-60% reduction in mortality and can reduce average stay time by 30% on average.21
On a smaller scale, self-administered connected medical devices can give doctors similar information, while also empowering patients with control over their own care. This is especially valuable when it comes to treating lifelong chronic conditions like diabetes 1. In the past, this condition required attentive monitoring of blood sugar levels and management of insulin administration. But today, devices like IoT-equipped continuous glucose monitors (CGM) and insulin pumps can make the process mostly hands off, automatically checking blood sugar levels, delivering predictively dosed medication, and organizing health data in an accessible way.22
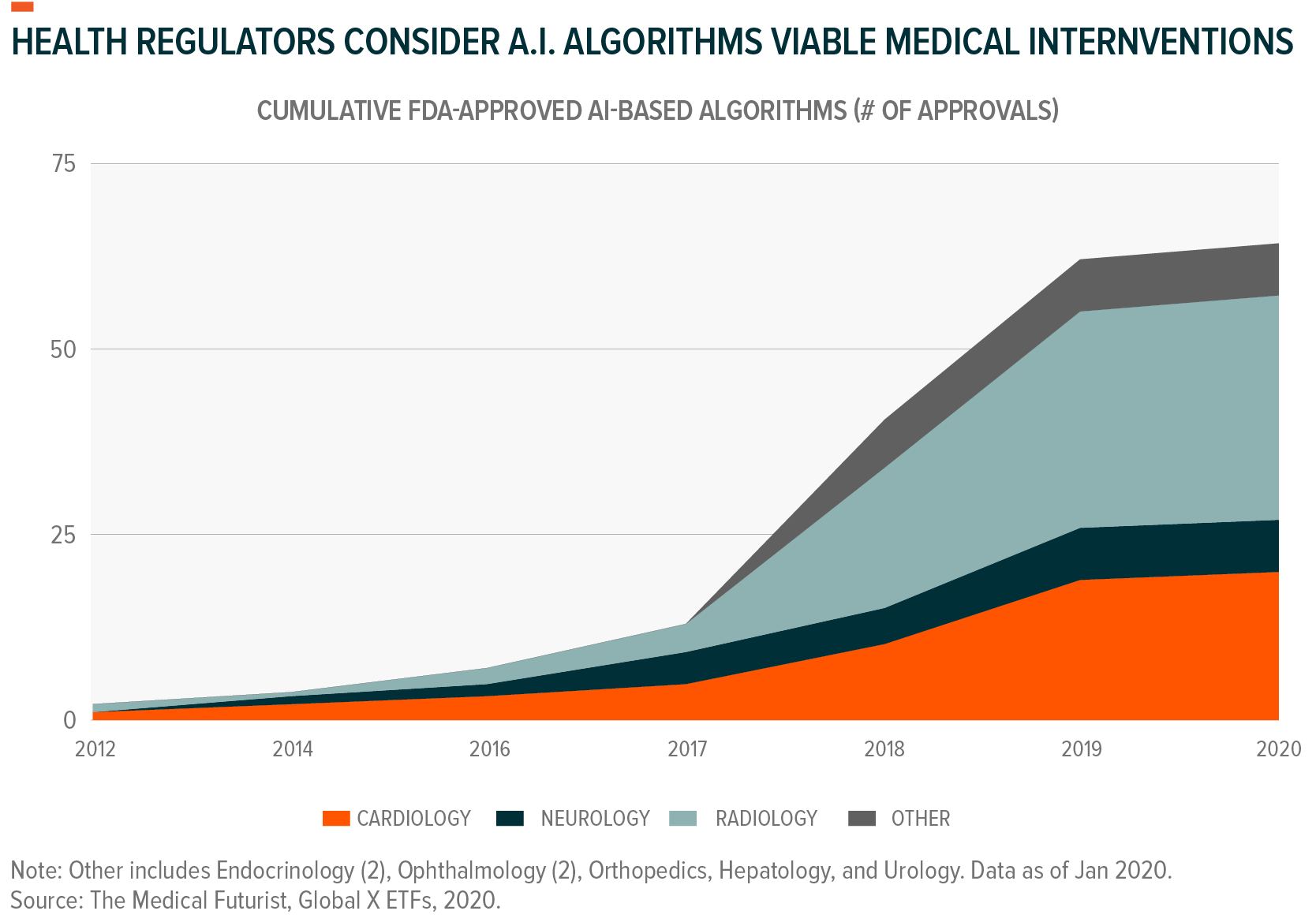
Data from these devices, health applications, and other sources can offer preventative health benefits when paired with genomic information and data from the broader health community. Artificial intelligence (AI) can put this data to use, finding patterns that can lead to precision treatments and smart diagnoses. By January 2020, the FDA approved over 60 different AI algorithms for medical treatment. These mostly included algorithms that analyze medical scans and images, including ones that characterize thyroid nodules, find lesions in the liver and lungs, and detect breast cancer with similar accuracy to that of radiologists.23
Conclusion
Telemedicine and Digital Health can expand access to health care by making it more geographically and financially accessible, presenting opportunities for large scale adoption. Additional opportunity lies in the technologies’ potential to revolutionize treatment options, improve patient outcomes, and streamline health care systems.
In our view, companies that offer services that connect physicians and patients over digital mediums will benefit from the rise of this theme, as will those that develop connected health care devices, operate in the health care analytics space, and/or the administrative digitization segment.